The Silent Aftermath of Surgery
Surgeons excel at repairing structural damage—whether it is mending a torn rotator cuff, replacing a knee joint, or performing a cesarean section. However, once the incision closes, the body’s natural biological repair process takes over. While this process is critical for survival, it often leaves behind a frustrating complication: Scar Tissue and Fascial Adhesions.
In orthopedic and post-operative rehabilitation, managing these adhesions is often the difference between regaining a full, pain-free range of motion (ROM) and being permanently restricted.
In recent years, highly trained Physical Therapists (PTs) and Occupational Therapists (OTs) have integrated a powerful tool into their scar-management protocols: Myofascial Decompression (Cupping).
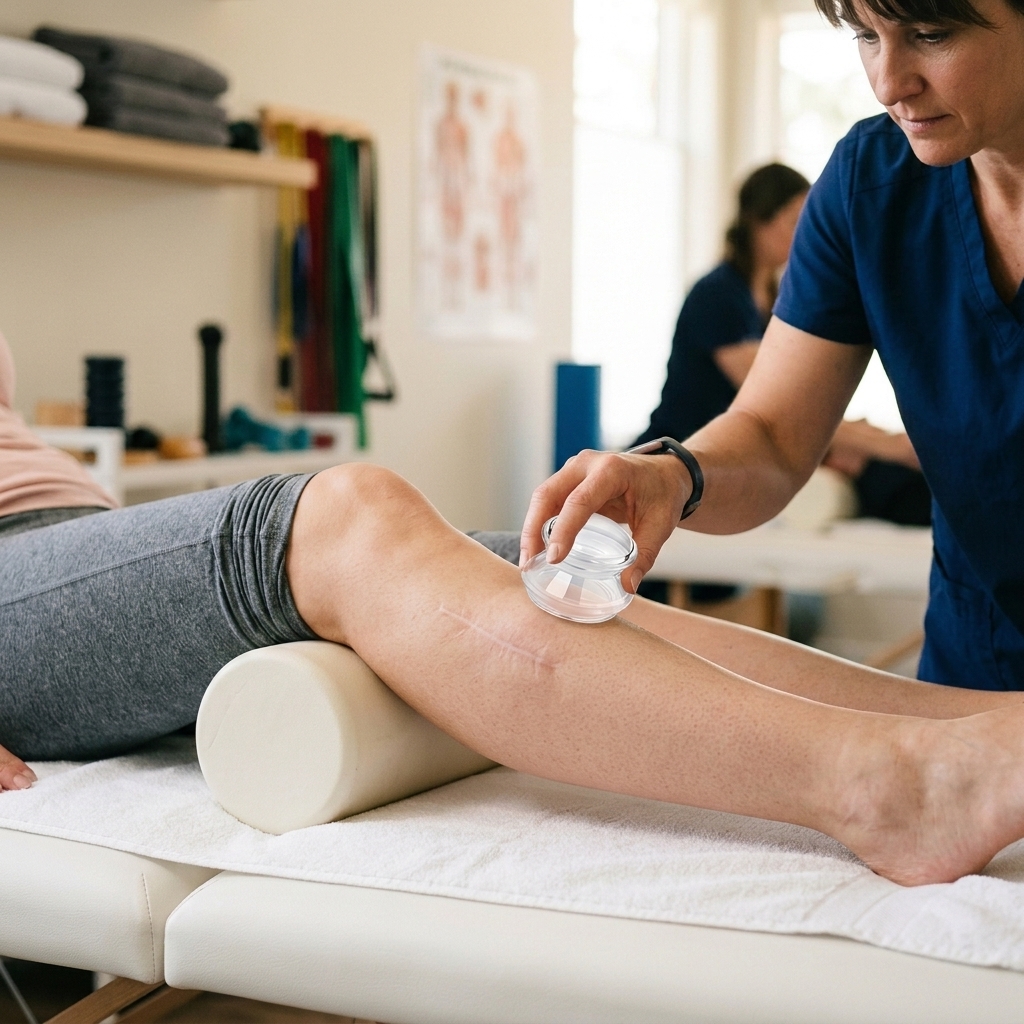
The Mechanics of a Scar
To understand why cupping is used, we must first understand what a scar is.
Healthy fascia and muscle fibers are highly organized, running in parallel lines that allow them to glide effortlessly over one another during movement. When the body repairs surgical trauma, it rapidly lays down collagen fibers. However, this new scar tissue is chaotic and disorganized—like a tangled web of rigid threads.
As this web matures, it often thickens and binds the skin, the superficial fascia, and the underlying muscle together into one solid block. This is a fascial adhesion. These adhesions act like internal superglue. They pull on surrounding tissues, restrict joint mobility, and trap superficial nerves, leading to chronic pinching and burning pain long after the original structural injury has healed.
How Suction Remodels Collagen
Attempting to break up mature scar tissue with traditional deep tissue massage (downward compression) can be incredibly painful and mechanically inefficient. You cannot simply "crush" an adhesion away.
Myofascial Decompression (Cupping) changes the mechanical vector. Here is the science behind how it remodels scar tissue:
1. Generating Vertical Shear Force
When a silicone cup is applied over or adjacent to a mature scar, the negative pressure vacuums the skin and superficial fascia upward. This upward lift creates a shearing force between the tissue layers. By physically pulling the skin away from the underlying tethered muscle, the cup gently micro-stretches and breaks the rigid, disorganized collagen cross-links that form the adhesion.
2. Restoring Viscoelasticity and Fluid Dynamics
Scars are dense and ischemic (lacking blood flow). The localized suction forcefully draws oxygen-rich blood, interstitial fluid, and lymphatic circulation into the dense, fibrous matrix. This hydration makes the thick tissue more pliable (viscoelastic), restoring its ability to stretch and glide during movement.
3. Neurological Desensitization
The skin surrounding a surgical scar is often hypersensitive due to trapped superficial nerve endings. The novel sensory input of gentle, sustained suction can stimulate mechanoreceptors in the skin, which helps downregulate (calm) the nervous system's heightened pain response in that specific area.
Why Glass Fails and Silicone Prevails
When treating sensitive post-operative tissue, precise control is not just a preference; it is a clinical necessity.
Traditional rigid glass or hard plastic pump cups are notoriously difficult to modulate. Furthermore, their hard, unyielding edges can dig painfully into hypersensitive scar tissue and are impossible to keep sealed over the complex contours of knees, shoulders, and abdomens.
This is exactly why rehabilitation clinics mandate the use of Medical-Grade Silicone Cupping Sets.
By using flexible silicone—like the classic mushroom body sets engineered by ELERACUPPING—therapists can instantly squeeze the cup to dial in the exact microscopic level of negative pressure a patient can tolerate. More importantly, the soft, pliable silicone edges allow the therapist to smoothly glide the cup over the bumpy, uneven terrain of a c-section or orthopedic scar without causing additional mechanical trauma to the skin.
⚠️ CRITICAL CLINICAL PRECAUTIONS & DISCLAIMER
Myofascial decompression for scar tissue must be approached with extreme caution and should ideally be guided by a licensed rehabilitation professional.
- Never Cup an Unhealed Wound: Cupping must NEVER be applied to fresh incisions, open wounds, or scars where the dermis is not fully closed and mature. Premature pulling can easily rip surgical sutures or staples, causing severe tissue damage and infection.
- Wait for Medical Clearance: Depending on the depth and location of the surgery, therapists typically wait a minimum of 6 to 12 weeks post-operation before applying direct negative pressure. Always secure clearance from the referring surgeon.
- Contraindications: Avoid cupping over deep vein thrombosis (DVT), active infections, or in patients with severe skin frailness (such as those on long-term corticosteroids).
Disclaimer: This article is strictly for educational purposes and does not constitute medical advice or a treatment protocol. Always consult a licensed healthcare provider before utilizing cupping therapy for post-surgical rehabilitation.
Safe, Professional-Grade Rehabilitation Tools
Discover why PTs and clinics trust ELERACUPPING's 100% Medical-Grade Platinum Silicone Sets for sensitive scar and fascial release protocols.
Discover Wholesale Silicone Sets